Possesses combined functionality and benefits of a cervical interbody and an anterior cervical plate.
TrellOss®-C SA Porous Ti Interbody System

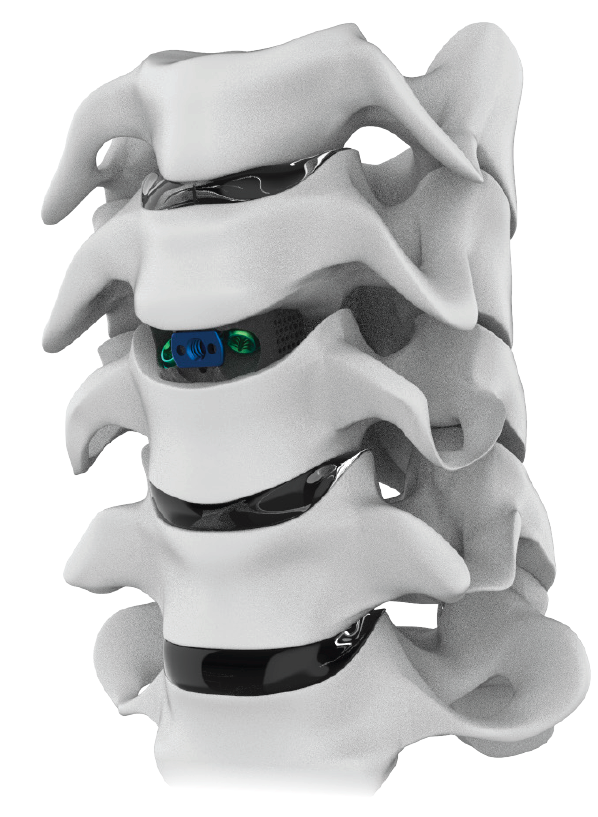
A New Foundation for Growth
The TrellOss-C SA Porous Ti Interbody System is a stand-alone anterior cervical interbody fusion system intended for use at one or two contiguous levels.
System Features
A 3D printed titanium interbody platform featuring a scaffold structure with 70% porosity and a 7 micron roughened surface topography to foster a cellular relevant environment for adhesion and bone ingrowth.1

Combined Functionality
- TrellOss-C SA possesses combined functionality and benefits of a cervical interbody and an anterior cervical plate.

Structure
- Scaffolding structure provides additional surface area 2,3 and an elastic modulus similar to PEEK.8
- Implant is contained within the region of the excised disc space and is designed to not protrude past the mid-line edge of the vertebral bodies, reducing the amount of soft tissue damage or irritation.

Sterile-packed
- Implants are sterile-packed for reduced risk of contamination and hospital reprocessing costs.

Texture
- Roughened surface provides initial stabilization and integrated turn lock allows for visual confirmation of locked position.
- 7 micron surface texturing enhances the wicking nature9 and creates an environment for potential cellular adhesion.2,3,4

Porosity
- Aligned pore structure allows optimal fluoroscopy when assessing fusion post-operatively.
- Open architecture with 70% porosity including varying pore sizes of 300, 500, and 700 microns that mimic cancellous bone allowing for a conducive environment for cellular activity.1,5,6,7

